 There has been a lot of discussion about the cost of new hepatitis C treatments to state Medicaid programs. What has not been addressed, however, is how those costs stack up against older, less effective treatments or the cost when Medicaid recipients with hepatitis C go untreated.
There has been a lot of discussion about the cost of new hepatitis C treatments to state Medicaid programs. What has not been addressed, however, is how those costs stack up against older, less effective treatments or the cost when Medicaid recipients with hepatitis C go untreated.
A series of new state-specific fact sheets from RxEconomics, LLC, in collaboration with PhRMA, detail the utilization of health services and the costs of treating Medicaid recipients with hepatitis C prior to the availability of new medicines to treat the disease. The analysis, which uses administrative claims data from 2010 provided by the Centers for Medicare and Medicaid Services, highlights the economic burden of treating Medicaid recipients with hepatitis C and the opportunity for newer and more effective medicines to lower health care costs with greater efficacy.
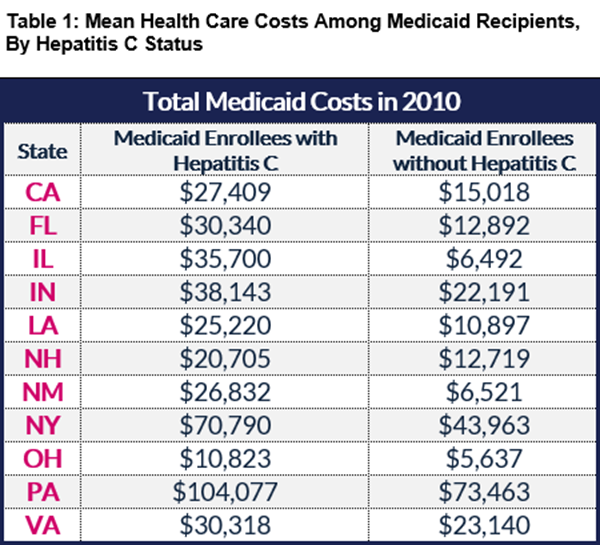
Prior to the availability of new hepatitis C medicines, the annual health care costs for Medicaid enrollees with the disease were, on average, substantially greater than enrollees without the disease (see Table 1).
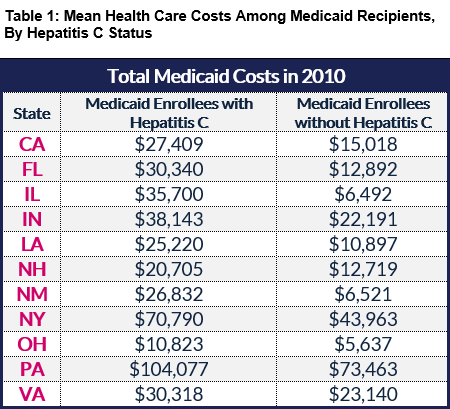
However, while patients who were treated with older medications, which offer cure rates of just 50 percent, incurred substantial prescription drug costs, untreated hepatitis C patients were still averaging significantly more in non-drug healthcare costs, especially as it related to inpatient hospitalizations (see Table 2).
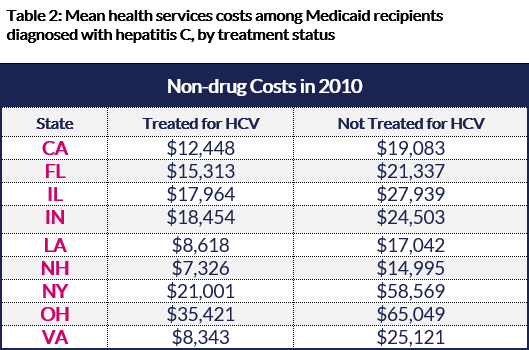
Compared to older treatments, this descriptive analysis provides early evidence to suggest that the new generation of hepatitis C medicines, which have cure rates of more than 90 percent, benefit patients and could potentially reduce the use and costs of some Medicaid services. Indeed, any assessment of the value of new hepatitis C treatments should take into account these medical cost offsets, as well as savings generating in replacing older, less effective medicines.
The fact sheets further underscore the importance of acknowledging the value that innovative treatments provide in managing long-term health care spending. As more patients receive access to these new medicines, experts have predicted that hepatitis C will become a rare disease within the next 20 years. On the other hand, in the absence of a cure for hepatitis C, more than 350,000 patients would be living with advanced stages of the disease by 2025 and Medicaid would incur additional spending of $21.5 billion.
Advances such as these exemplify the integral role that medicines play in not only helping patients live healthier, more productive lives, but also preventing economic burdens and relieving stress on the health care system. In the absence of effective treatments, we would be living in a far different world than we do today.


 There has been a lot of discussion about the cost of new hepatitis C treatments to state Medicaid programs. What has not been addressed, however, is how those costs stack up against older, less effective treatments or the cost when Medicaid recipients with hepatitis C go untreated.
There has been a lot of discussion about the cost of new hepatitis C treatments to state Medicaid programs. What has not been addressed, however, is how those costs stack up against older, less effective treatments or the cost when Medicaid recipients with hepatitis C go untreated.

